- Find a Doctor
- Appointments and Second Opinions
- Find a Location
- Patient Portals

Department of Medical Oncology

The Department of Medical Oncology provides compassionate clinical care for patients with cancer; conducts transformative basic, translational, and clinical research; and provides leading education, training, and mentorship in cancer medicine.
Clinical, Research, and Educational Activities

Patient Care
Integration of clinical care and research, with a personalized and multidisciplinary approach to oncology medicine

Basic research focused on blood and solid tumors, molecular and cellular oncology, and population sciences

The department coordinates hematology and oncology fellowships at Brigham and Women's Hospital, Dana-Farber, and Massachusetts General Hospital, and offers clerkships in hematology/oncology at Harvard Medical School.
Medical Oncology By the Numbers
- 300+ Harvard Medical School (HMS) Faculty
- 360+ Clinical and Research Fellows
- $280M+ Research dollars awarded to our investigators in 2022
Our Patient Care
- 14 Clinical divisions led by Internationally recognized leaders in their fields
- 290,000+ outpatient visits in 2022
- 190+ average inpatient daily census
Our Research
- 3 Research divisions creating academic communities of investigators with similar interests
- 80+ highly collaborative research labs
- 637 Clinical trials in Fiscal Year 2022
Medical Oncology at Dana-Farber
Trace the remarkable growth and development of medical oncology at Dana-Farber – from its early roots to today’s mission-driven commitment to excellence in research, care, collaboration, and training.
Research and Care Within — and Across — Disease Boundaries
The Department of Medical Oncology integrates outstanding basic cancer research and clinical oncology within the same department. Clinician-scientists within Medical Oncology provide substantial expertise within their specific programs, as well as interdisciplinary areas such as cancer genetics and prevention, early drug development, and population sciences.
Clinicians in the department have deep understanding of the genetics and biology of cancer and engage in clinical research with deep correlative scientific studies. Nearly all basic scientists in the department are clinically trained and are motivated to link the implications of laboratory findings to potential clinical impact, and to take clinical observations as the inspiration for laboratory studies. Nearly all laboratory-based principal investigators also see patients in a clinical division, and many attend on inpatient services. And most clinical investigators have ties to one or more research or disease programs within Dana-Farber/Harvard Cancer Center (DF/HCC).
All of our faculty collaborate with external institutions and serve on national and international oncology committees and steering groups. Faculty actively contribute service and leadership, providing an open two-way conduit for expertise that benefits the Institute and the broader oncology and health care communities. Faculty perform cutting-edge basic and clinical research, and provide education and training to the next generation of physicians and scientists who are focused on the biology and treatment of cancer.
Support Our Cancer Research
To learn more about the many ways you can support Dana-Farber's research initiatives with a philanthropic gift, please email Rebecca Shortle or call 617-632-4215
Recent Topics in Medical Oncology at Dana-Farber

- Utility Menu
GA4 tracking code

Cancer Program
Researchers in the hsci cancer program are working to establish the crucial differences between normal stem cells and their cancerous counterparts..
The goal of the program is to develop therapies that can eradicate cancer cells – and their entire lineage – without harming healthy tissues. This ambitious goal demands a profound understanding of how, precisely, a normal stem cell becomes a cancer cell. Some of the world’s foremost cancer researchers are collaborating across Harvard's schools and hospitals to do just that.
- Identify the critical genes and pathways that distinguish cancer from normal stem cells.
- Pinpoint which of these – in what combination – could serve as candidate targets for therapy.
What we have achieved so far:
HSCI Cancer Program scientists have:
- Isolated normal stem cell populations from intestine and colon tissue, and characterised their molecular profiles extensively.
- Identified and investigated key pathways operating in lung-tumor-propagating cells.
- Demonstrated what factors are required for leukemia stem cell development and survival.
- Clarified the role of a specific mutation that controls signaling in tumor-propagating cells in human pancreatic tumors.
- Developed imaging technologies for visualizing single tumor-initiating stem cells in the laboratory.
Program Leaders:

Carla F. Kim, Ph.D.

Mario Suva, M.D., Ph.D.
Get the latest hsci research news, related news, mutant protein switches sides in melanoma, kara mckinley named packard fellow for science and engineering, kara mckinley receives nih director’s new innovator award, hsci faculty member appointed the inaugural regenerative biology endowed chair at boston children’s hospital.
- Blood Program
- Cardiovascular Program
- Diabetes Program
- Kidney Program
- Nervous System Diseases Program
- Musculoskeletal Program
- Skin Program
- Aging & Fibrosis
- Stem Cells as Tools
- Early-Stage Research
- For Patients

DF/HCC Is a Research Consortium
that provides shared resources and a collaborative environment for over 1,100 cancer researchers at 7 Harvard institutions. Learn more about DF/HCC here

Information for DF/HCC members and collaborators

Shared resources available to DF/HCC members

Resources and initiatives for Massachusetts communities
Opportunities for training and career enhancement
Clinical Investigator Support and Trial Search Tool

Center Funding & Announcements
September 24, 2024 – Announcements
Funding opportunity for NCI Early Career Cancer Clinical Investigator Award
NCI is requesting applications for the Early Career Cancer Clinical Investigator Award (ECIA). The ECIA recognizes and supports outstanding early career clinical investigators who are committed to building a career as an…
September 24, 2024 – Cancer Disparities
Faces of Faith
Faces of Faith is on exhibit September 23 - November 1; In-Person RECEPTION: OCTOBER 15, 2024 | 4:00 PM EST
September 17, 2024
Announcing Nareg Grigorian as new Director, Office of Data Quality (ODQ)
We are pleased to announce that Nareg Grigorian has been named as the new Director, Office of Data Quality supporting clinical research across Dana-Farber/Harvard Cancer Center. Nareg’s many years of service, and his…
September 17, 2024 – Announcements
Mentorship in Clinical and Translational Research
A guide to empower mentees and mentors in maximizing their mentoring relationships and growing their networks.
Event Highlights
- Sep 26 Defining the Data Ecosystem for a Cancer Learning Health Systems
- Sep 27 Defining the Data Ecosystem for a Cancer Learning Health Systems
Featured Topics
Featured series.
A series of random questions answered by Harvard experts.
Explore the Gazette
Read the latest.

Suicide among female doctors gets a closer look

Eat this. Take that. Get skinny. Trust us.

High doses of Adderall may increase psychosis risk
To assess a smoker’s lung cancer risk, think years — not packs.
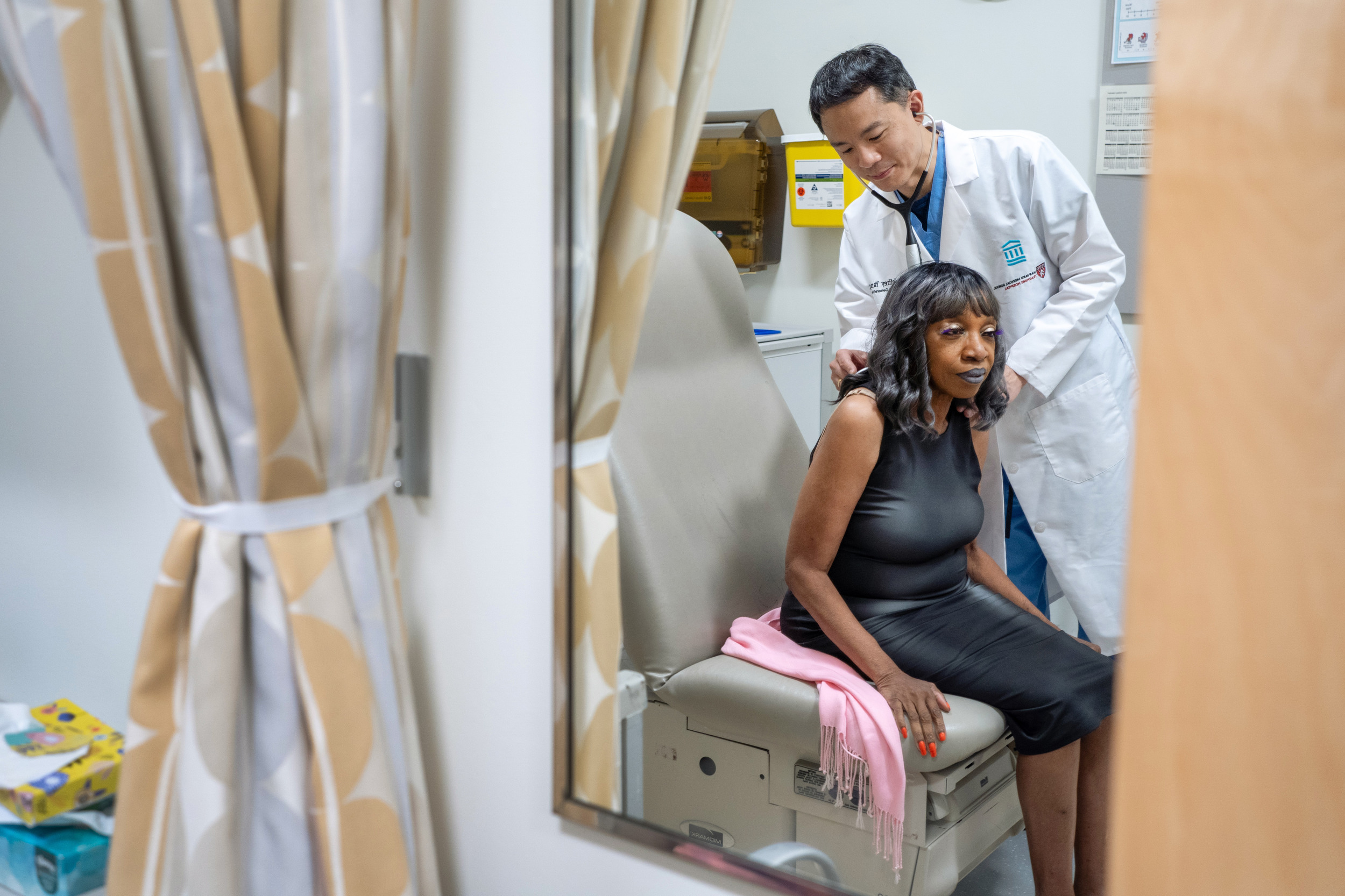
Jeffrey Yang with patient Albertha Gethers, who was treated for lung cancer at Mass General Hospital.
Photos by Jodi Hilton; Illustrations by Liz Zonarich/Harvard Staff
Alvin Powell
Harvard Staff Writer
Far more cases get caught when screening guidelines consider duration of habit regardless of intensity, study finds — especially among Black patients
When deciding who to screen for America’s deadliest cancer, should a person who has smoked a pack a day for 20 years get priority over someone who has smoked fewer cigarettes over the same amount of time?
That’s the question tackled by Harvard Medical School and Massachusetts General Hospital researchers in a recent study that showed that lung cancer screening guidelines set by the U.S. Preventive Services Task Force — requiring the equivalent of a pack a day for 20 years — miss a large proportion of cases and fail to close a screening gap between Black and white patients. That gap means lung cancer among Black patients is too often caught later in the disease’s course, leading to higher mortality.
The researchers, whose work was published earlier this year in the Journal of Clinical Oncology , suggest switching instead to a simple measure that would recommend annual screening for anyone who’s smoked for 20 years, regardless of how many cigarettes they smoke a day. Both guidelines also require the individuals be between ages 50 and 80 and either be current smokers or having quit within the last 15 years. The simplified guideline would widen the pool of those who qualify for lung cancer screening and, according to the study, both increase the proportion of cancer cases that are caught and virtually eliminate racial disparities in lung cancer screening eligibility.
“We found that it completely eliminated the racial disparity in the proportion of lung cancer patients who would have qualified among both people who currently smoke as well as people who formerly smoked,” said Alexandra Potter , the study’s first author, clinical research coordinator at Massachusetts General Hospital, and president of the American Lung Cancer Screening Initiative .

Smoking duration vs. intensity and risk
The 20 pack-year threshold can be difficult to use and inaccurate, said senior author Chi-Fu Jeffrey Yang , associate professor of surgery at Harvard Medical School and a thoracic surgeon at MGH. That’s because the equivalent of smoking a pack a day for 20 years could mean smoking half a pack daily for 40 years, two packs a day for 10, or any other permutation that results in the required combination of smoking intensity and duration. In addition, most people who smoke have smoked different amounts at different times of their lives which, decades later, can be difficult to recall. Plus, while it may make intuitive sense that someone who smokes more intensely has a higher risk of developing lung cancer, studies have not shown that the risk due to smoking intensity is equivalent to the risk from smoking duration, as the pack-year standard implies, the authors said.
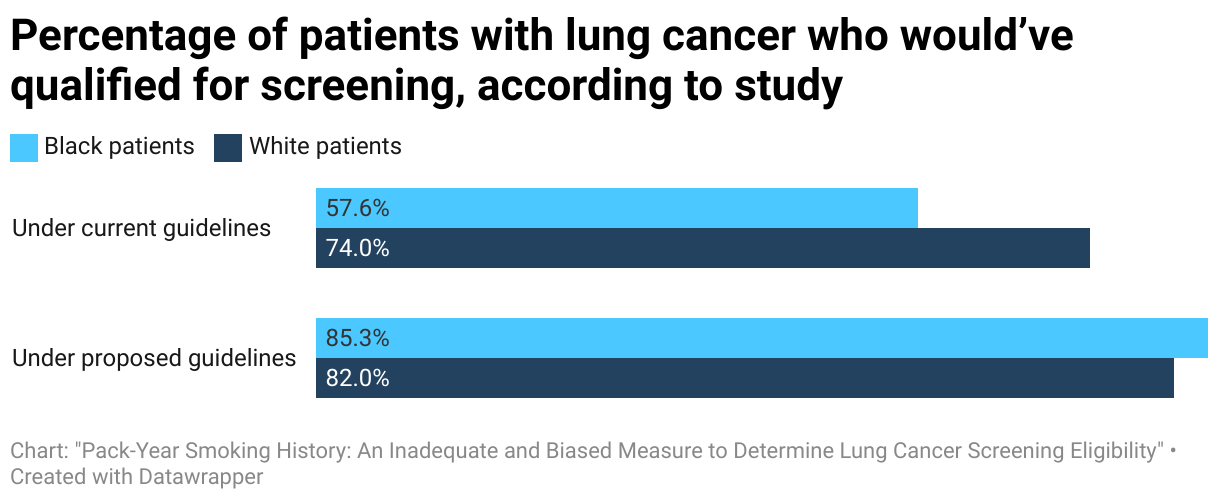
White patients tend to smoke more each day
In the work, supported by the National Institutes of Health and the Agency for Healthcare Research and Quality, researchers applied both the current screening guidelines and the proposed simplified guidelines to participants in two studies: the Southern Community Cohort Study, which included both Black and white subjects receiving care at community health centers in the U.S. Southeast, and the Black Women’s Health Study, whose study population was limited to Black women. Both included data on subjects’ health and smoking history.
Researchers first applied the current screening guideline and found that, of those who developed lung cancer in the Southern Community Cohort Study, just 58 percent of Black patients and 74 percent of white patients would have qualified for screening. In the Black Women’s Health Study, just 43 percent of those who developed lung cancer would have qualified for screening.
By contrast, applying the simplified 20-year smoking duration guideline would capture over 80 percent of both Black and white participants who developed lung cancer in the Southern Community Cohort Study, and 64 percent of lung cancer patients in the Black Women’s Health Study. That would not only significantly increase the percentage of lung cancer cases eligible for screening, it would virtually eliminate the racial disparity in eligibility.
That racial disparity, the authors said, largely stems from the fact that current guidelines include the pack-a-day measure of smoking intensity, which varies between Black and white individuals. White individuals smoke significantly more each day, lowering the bar for screening eligibility. That has been seen in previous studies and was apparent in Potter and Yang’s research as well. Research has identified several possible explanations for differences in smoking intensity and lung cancer risk, including differences in nicotine metabolism between Black and white people who smoke. However, there are also an array of social and cultural factors still unexplored, the authors said.
“We showed that the median number of cigarettes smoked among Black patients with lung cancer was almost half of that among white patients with lung cancer,” Potter said. “Even though they smoke similar durations, intensity was really the driving factor in the difference between them.”
Other screening barriers
The debate over who should get screened and when is just one part of lung cancer’s dismal landscape. Smoking is its leading cause, accounting for 85 percent of cases. It is one of the most aggressive cancers, Yang said, meaning it can spread rapidly if not caught early. It kills more people annually — in both the U.S. and the world — than colon, breast, and prostate cancers combined, and is expected to kill 125,070 Americans in 2024, according to statistics from the American Cancer Society.
Despite lung cancer’s deadly record, a recent study by the American Lung Association showed that more than 80 percent of those who qualify for screening don’t even know it is an option. Further, only between 5 percent and 19 percent of those who qualify actually get screened for lung cancer.
“It pales in comparison to breast cancer, colon cancer, and cervical cancer screening, where 70 to 80 percent get screened,” Yang said. “There’s a huge gap.”
Of those who qualify for lung cancer screening don’t even know it’s an option

Of those who qualify actually get screened for lung cancer

Of lung cancer cases are caused by smoking

Americans are expected to die from lung cancer this year
In addition to lack of awareness, part of that gap may be due to additional requirements placed on those seeking a lung cancer screening, Potter said. Unlike a mammogram, which a patient can schedule themselves, lung cancer screening has to be scheduled in conjunction with a visit to a healthcare provider. While it’s not bad to have a provider involved, Potter said, it is an extra step and one required by many insurers before they’ll pay for the procedure.
“Out of lung, breast, colon, and cervical cancer, lung cancer is the only one where it’s required to have this formal documentation of a shared decision-making visit,” Potter said.
The screening itself is straightforward, noninvasive, and takes just minutes, Yang said. Patients can stay in their street clothes and lie on a table for a CT scan that takes a series of X-rays to create an image of the lungs, revealing any tumors that might be present.
Yang said a recent patient’s case highlights the situation. She smoked lightly — just three cigarettes a day — but for many years. The light intensity of her habit put her at just 8.4 pack-years, not enough to qualify for lung cancer screening. Fortunately, she was able to get screened through an ongoing clinical trial, called INSPIRE, that Potter and Yang are leading to investigate lung cancer screening in high-risk Black women. The scan showed three small, aggressive cancerous nodules that Yang was able to remove surgically.
“She’s doing very well right now, but she’s 69 and without the screening this would certainly have come back in her 70s as stage IV lung cancer with a very, very different outcome,” Yang said. “We’re hoping that people take a good look at pack-years and whether this is really the best measure overall and the best criterion for Black cancer screening eligibility.”
Share this article
You might like.
Epidemiologist discusses research, shrinking gap between rates of male, female physicians, what can be done

Popularity of newest diet drugs fuel ‘dumpster fire’ of risky knock-offs, questionable supplements, food products, experts warn

Among those who take prescription amphetamines, 81% of cases of psychosis or mania could have been eliminated if they were not on the high dose, findings suggest
Good genes are nice, but joy is better
Harvard study, almost 80 years old, has proved that embracing community helps us live longer, and be happier
Do phones belong in schools?
Banning cellphones may help protect classroom focus, but school districts need to stay mindful of students’ sense of connection, experts say.
- U.S. Department of Health & Human Services

- Virtual Tour
- Staff Directory
- En Español
You are here
News releases.
Media Advisory
Tuesday, September 24, 2024
New cancer diagnoses did not rebound as expected following pandemic
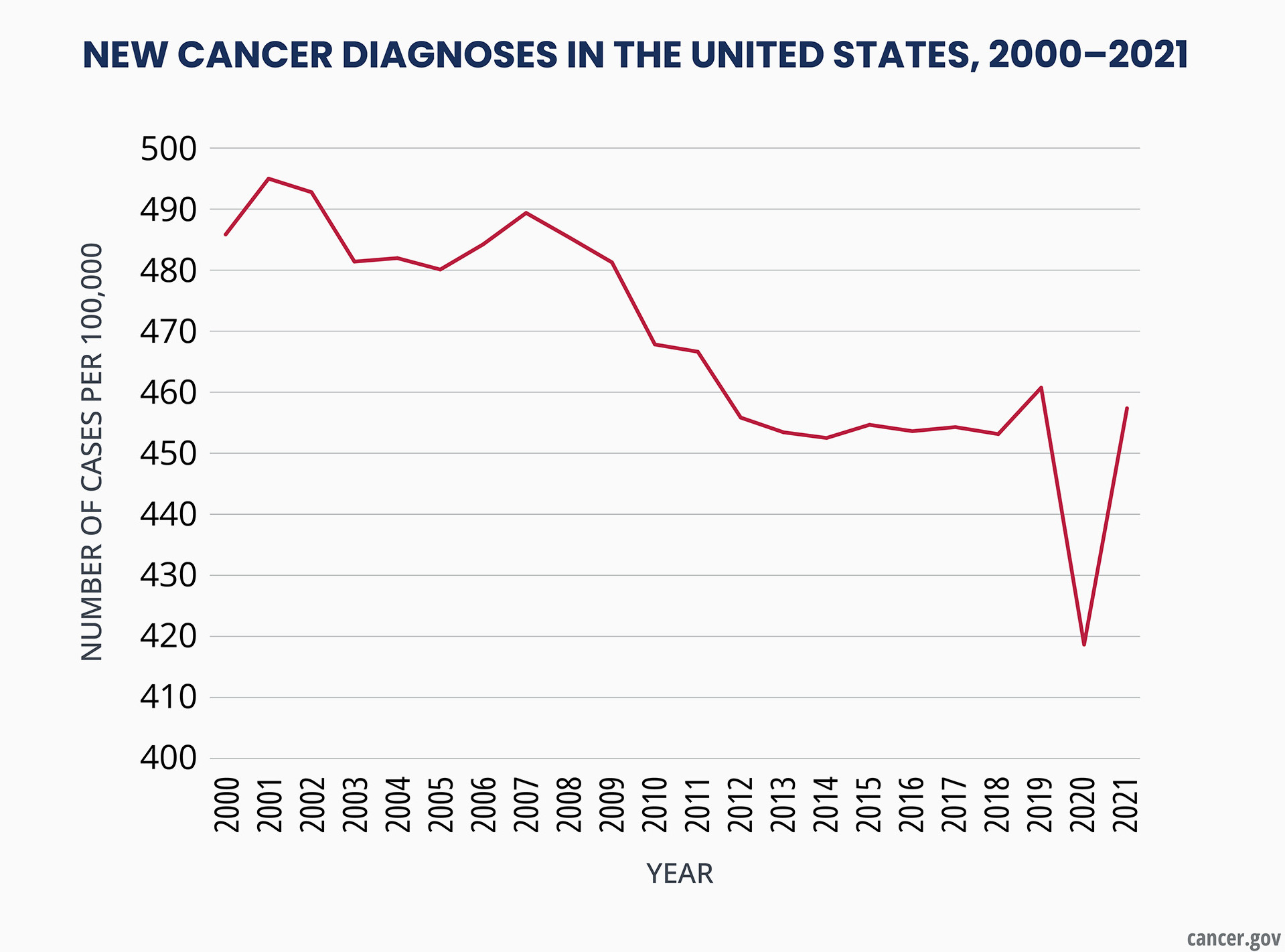
Cancer incidence trends in 2021 largely returned to what they were before the COVID-19 pandemic, according to a study by researchers at the National Institutes of Health (NIH). However, there was little evidence of a rebound in incidence that would account for the decline in diagnoses in 2020, when screening and other medical care was disrupted. One exception was breast cancer, where the researchers did see an uptick in diagnoses of advanced-stage disease in 2021. The study appears Sept. 24, 2024, in the Journal of the National Cancer Institute.
A previous study showed that new cancer diagnoses fell abruptly in early 2020, as did the volume of pathology reports, suggesting that many cancers were not being diagnosed in a timely manner. To determine whether these missed diagnoses were caught in 2021, possibly as more advanced cancers, researchers from NIH’s National Cancer Institute (NCI) compared observed cancer incidence rates for 2021 with those expected from pre-pandemic trends using data from NCI’s Surveillance, Epidemiology, and End Results Program .
A full recovery in cancer incidence should appear as an increase over pre-pandemic levels (also known as a rebound) to account for the missed diagnoses. The researchers looked at cancer overall, as well as five major cancer types that vary in how they are typically detected: through screening (female breast and prostate cancer), due to symptoms (lung and bronchus and pancreatic cancer), or incidentally during other medical procedures (thyroid cancer).
Cancer incidence rates overall and for most specific cancers approached pre-pandemic levels, with no significant rebound to account for the 2020 decline. However, in addition to an uptick in new diagnoses of advanced breast cancer in 2021, the data also provided some evidence of an increase in diagnoses of advanced pancreatic cancer. Also, new diagnoses of thyroid cancers in 2021 were still below pre-pandemic levels.
The researchers concluded that 2021 was a transition year that was still affected by new variants and new waves of COVID-19 cases, which continued to impact medical care. They said the findings highlight the need for ongoing monitoring to understand the long-term impacts of the pandemic on cancer diagnoses and outcomes.
Nadia Howlader, Ph.D., Division of Cancer Control and Population Sciences, National Cancer Institute
“ Impact of COVID-19 on 2021 Cancer Incidence Rates and Potential Rebound from 2020 Decline ,” appears September 24, 2024, in the Journal of the National Cancer Institute.
About the National Cancer Institute (NCI): NCI leads the National Cancer Program and NIH’s efforts to dramatically reduce the prevalence of cancer and improve the lives of cancer patients and their families, through research into prevention and cancer biology, the development of new interventions, and the training and mentoring of new researchers. For more information about cancer, please visit the NCI website at cancer.gov or call NCI’s contact center, the Cancer Information Service, at 1-800-4-CANCER (1-800-422-6237).
About the National Institutes of Health (NIH): NIH, the nation's medical research agency, includes 27 Institutes and Centers and is a component of the U.S. Department of Health and Human Services. NIH is the primary federal agency conducting and supporting basic, clinical, and translational medical research, and is investigating the causes, treatments, and cures for both common and rare diseases. For more information about NIH and its programs, visit www.nih.gov .
NIH…Turning Discovery Into Health ®
Connect with Us
- More Social Media from NIH

COMMENTS
The new Damon Runyon-St. Jude Pediatric Cancer Research fellowships support innovative projects in basic or translational research that have potential to significantly improve the diagnosis or treatment of one or more pediatric cancers. Each fellowship provides funding for four years, totaling $300,000.
It's become clear that tumors can modify their own genes to evade detection and attack by the immune system. A new study in mice reveals how these changes happen and identifies for the first time a comprehensive list of the genes affected.The work, led by Harvard Medical School researchers at Beth Israel Deaconess Medical Center and Boston Children's Hospital, provides a roadmap for ...
Innovation fuels discovery at Harvard Medical School, where more than 11,000 faculty members and over 1,600 medical and graduate students strive to alleviate suffering caused by disease. This work takes place on the School's Boston campus and across the metropolitan area at 15 affiliated hospitals and research institutes.
To learn more about the many ways you can support Dana-Farber's research initiatives with a philanthropic gift, please email Rebecca Shortle or call 617-632-4215. The Department of Medical Oncology at Dana-Farber Cancer Institute offers comprehensive clinical and educational programs. Discover our innovative approach.
The work was in part supported by the National Institute of General Medical Sciences grant R35GM142879, the Department of Defense Peer Reviewed Cancer Research Program Career Development Award HT9425-23-1-0523, a Google Research Scholar Award, a Harvard Medical School Dean's Innovation Award, and a Blavatnik Center for Computational Biomedicine ...
About DF/HCC. Dana-Farber/Harvard Cancer Center (DF/HCC), an NCI-designated comprehensive cancer center, was founded to integrate and build upon the collective talent and resources of the Harvard cancer research community. Five Boston academic medical institutions—Beth Israel Deaconess Medical Center, Boston Children's Hospital, Brigham and ...
The work was in part supported by the National Institute of General Medical Sciences grant R35GM142879, the Department of Defense Peer Reviewed Cancer Research Program Career Development Award HT9425-23-1-0523, the Google Research Scholar Award, the Harvard Medical School Dean's Innovation Award, and the Blavatnik Center for Computational ...
Harvard Medical School (68) Harvard School of Dental Medicine (2) Harvard John A. Paulson School of Engineering and Applied Sciences (3) Harvard T. H. Chan School of Public Health (2) Harvard-MIT Division of Health Sciences and Technology (1) Howard Hughes Medical Institute (4) Joslin Diabetes Center (6) Massachusetts Eye and Ear (1)
HMS affiliates are advancing our understanding of cancer to improve human health. A detailed analysis of lung tumors that became resistant to targeted drugs has revealed two previously unreported resistance mechanisms. In the March 23 Science Translational Medicine, investigators from Massachusetts General Hospital Cancer Center and HMS also ...
HSCI Cancer Program scientists have: Isolated normal stem cell populations from intestine and colon tissue, and characterised their molecular profiles extensively. Identified and investigated key pathways operating in lung-tumor-propagating cells. Demonstrated what factors are required for leukemia stem cell development and survival.
These advances are delivering useful, productive changes that lead to better cancer outcomes. High-Impact Cancer Research is the acclaimed Harvard Medical School postgraduate certificate program for cancer research. It teaches the principles and skills shaping today's most important cancer research activities.
Cancer Cell Biology Program. The DF/HCC Cancer Cell Biology Program utilizes molecular, biochemical, and cell-based approaches to better understand cancer pathogenesis and to apply this knowledge to cancer therapeutics. The Program facilitates collaborations that funnel basic discoveries into the clinic or mine observations made in the clinic ...
People of Harvard Medical School; Research Departments, Centers, Initiatives and more. Research. ... Dana-Farber/ Harvard Cancer Center. Harvard Catalyst | The Harvard Clinical & Translational Science Center ... Harvard University Center for AIDS Research. HMS Division of Emergency Medicine.
Department of Pathology Research Faculty - BWH, MGH, BIDMC, BCH Disciplines Cancer Jon C. Aster, M.D., Ph.D., Professor of Pathology, Brigham and Women's Hospital ...
Q&A with Dr. George Demetri, High-Impact Cancer Research program co-directorDr. George Demetri, co-director of the Harvard Ludwig Center, HMS professor of medicine at Dana-Farber Cancer Institute, and a co-director of HMS High-Impact Cancer Research, answers popular questions about the program.
The Program seeks to reduce breast cancer morbidity and mortality by promoting transdisciplinary basic, translational, and clinical research within the DF/HCC community. The program fosters work that focuses on risk identification, prevention, treatment, and survivorship. Its hallmark is translational research, optimized by a web of ...
Main: (617) 632-3000. Spanish Speakers: (617) 632-3673. Visit Website. Dana-Farber/Harvard Cancer Center (DF/HCC) is a collaboration between academic institutions, world-renowned for its leadership in adult and pediatric cancer treatment and research. Dana-Farber Cancer Institute is a founding member of DF/HCC, established in Boston in 1947 ...
Understanding how immune cells recognize and kill cancer cells, and what we can do to enhance their ability to fight cancer, is important for anyone working to develop new cancer treatments or apply them in the clinic. This advanced course offers a unique way for professionals to learn about cutting-edge cancer immunotherapies from leading ...
The research is reported in Nature Biomedical Engineering. "Our approach is the exact opposite of conventional cancer treatments that focus on getting the immune system to recognize and attack the primary tumor, because those tumors are often large and difficult for immune cells to penetrate," said co-first author Zongmin Zhao, a ...
The Dana-Farber Cancer Institute, a prestigious Harvard teaching school, is moving to retract six studies and correct 31 others following allegations of data manipulation.
Harvard Medical School's High-Impact Cancer Research program strives to bridge the gap that exists between the science and business sectors when it comes to cancer research, creating a global network of experts. This postgraduate certificate program brings together high-level researchers, physicians, top-flight venture capitalists ...
Harvard Medical School. Dept. of Cell Biology, LHRRB 301A. 240 Longwood Avenue. Boston, MA 02115. Lab phone: 617-432-6865. Lab fax: 617-432-6932
Clinical Investigator Support and Trial Search Tool. Who are you? Central Administration. 450 Brookline Avenue, BP332A. Boston, MA 02215. (617) 632-2100. (877) 420-3951 Toll Free. (617) 632-4452 Fax. EMAIL.
The Raghavan Lab at Dana-Farber Cancer Institute and Harvard Medical School is a basic and translational oncology lab focused on understanding mechanisms of cell state regulation in cancer, evaluating how cell state plasticity influences therapeutic...
Eliz Amar Lewis has always been fascinated by biology. But when she saw her grandmother bravely battle breast cancer, she was inspired to use her passion to develop a smart and sophisticated therapeutic platform to fight such a complex disease. Now, she's part of a collaborative, multidisciplinary team developing an RNA-based cancer immunotherapy platform funded by ARPA-H.
That's the question tackled by Harvard Medical School and Massachusetts General Hospital researchers in a recent study that showed that lung cancer screening guidelines set by the U.S. Preventive Services Task Force — requiring the equivalent of a pack a day for 20 years — miss a large proportion of cases and fail to close a screening gap ...
Cancer incidence trends in 2021 largely returned to what they were before the COVID-19 pandemic, according to a study by researchers at the National Institutes of Health (NIH). However, there was little evidence of a rebound in incidence that would account for the decline in diagnoses in 2020, when screening and other medical care was disrupted.
Nadia Howlader, Ph.D., Division of Cancer Control and Population Sciences, National Cancer Institute. The Study "Impact of COVID-19 on 2021 Cancer Incidence Rates and Potential Rebound from 2020 Decline," appears September 24, 2024, in the Journal of the National Cancer Institute.